ARDMS AE Adult Echocardiography Examination AE-Adult-Echocardiography Exam Questions
When should the left ventricular end-diastohc diameter be measured?
Answer : B
Comprehensive and Detailed Explanation From Exact Extract:
The left ventricular end-diastolic diameter (LVEDD) is measured at end-diastole, which is conventionally defined as the onset of the QRS complex on the electrocardiogram (ECG). This corresponds to the end of ventricular filling and just before ventricular contraction begins.
Measuring LVEDD at this point ensures consistency and accuracy for assessment of ventricular size and function. Measurement at the onset of the P wave would be too early (atrial contraction). The first frame after aortic valve closure corresponds to end-systole, and after mitral valve closure is during systole.
This timing is standard as per guidelines outlined in the 'Textbook of Clinical Echocardiography, 6e', Chapter on Cardiac Chamber Quantification20:60-65Textbook of Clinical Echocardiography.
Which is the most likely abnormality represented in these images from a 48-year-old man with shortness of breath?
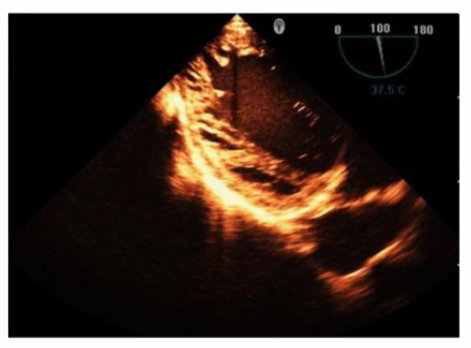
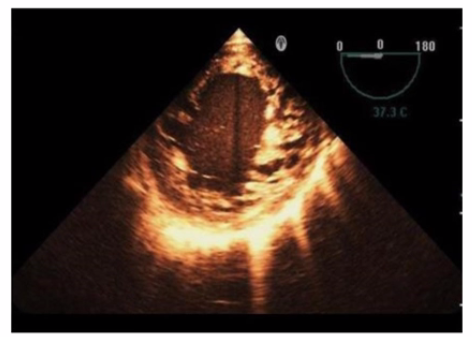
Answer : C
The echocardiographic images show prominent trabeculations and deep intertrabecular recesses communicating with the left ventricular cavity, best seen on contrast-enhanced images. This finding is characteristic of left ventricular noncompaction (LVNC), a cardiomyopathy resulting from arrested myocardial compaction during embryogenesis.
LVNC is diagnosed by visualizing a two-layered myocardium with a thin compacted epicardial layer and a thicker noncompacted endocardial layer with deep trabecular recesses. The use of contrast echocardiography enhances endocardial border delineation and recess visualization, increasing diagnostic accuracy.
Loeffler syndrome (hypereosinophilic cardiomyopathy) often shows endomyocardial fibrosis and restrictive physiology but not prominent trabeculations. Hypertrophic cardiomyopathy shows asymmetric septal hypertrophy without deep recesses. Ischemic cardiomyopathy shows wall motion abnormalities but not characteristic trabecular patterns.
These diagnostic criteria and imaging features are well documented in the 'Textbook of Clinical Echocardiography' and ASE guidelines on cardiomyopathies and use of contrast echo16:Textbook of Clinical Echocardiography, 6eChapter on LV Noncompaction12:ASE Contrast Echocardiography Guidelinesp.180-190.
Which procedure is most appropriate for evaluation of an atrial septal defect in the presence of an atrial septal aneurysm?
Answer : D
Transesophageal echocardiography (TEE) provides superior visualization of the atrial septum, especially in the presence of an atrial septal aneurysm, which may obscure transthoracic views. TEE allows detailed anatomic assessment of the atrial septal defect (ASD), its size, and associated structures.
Agitated saline contrast echo is useful for detecting right-to-left shunts but is limited in anatomical delineation in complex cases. Cardiac MRI and catheterization can provide complementary information but are not first-line for ASD evaluation when TEE is available.
ASE adult congenital heart disease guidelines and echocardiography texts emphasize TEE as the gold standard for ASD evaluation in this setting12:ASE Adult Congenital Guidelinesp.405-41016:Textbook of Clinical Echocardiography, 6ep.570-575.
Which flow component is indicated by the arrows on this image?
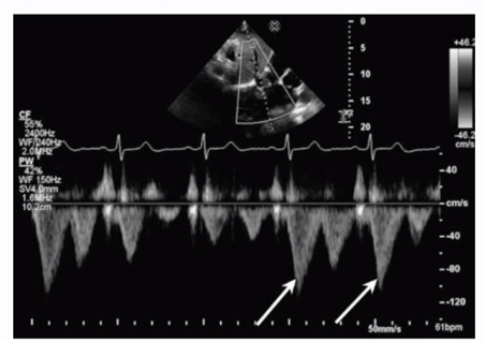
Answer : C
The Doppler waveform shows pulmonary vein flow with several components. The arrows point to small reversed flow spikes just after the atrial contraction wave, which corresponds to the atrial reversal (AR) flow component. Atrial reversal occurs as blood briefly flows backward into the pulmonary veins during atrial contraction.
Ventricular reversal is not typically seen in pulmonary veins. Diastolic flow reversal is abnormal and usually not part of normal pulmonary vein flow. Systolic forward flow is the major forward component during ventricular systole.
This interpretation is standard in ASE guidelines on diastolic function assessment and pulmonary vein Doppler evaluation12:ASE Diastolic Function Guidelinesp.85-9016:Textbook of Clinical Echocardiography, 6ep.130-135.
Which statement is most accurate regarding cardiac contusion?
Answer : A
Cardiac contusion is a myocardial injury resulting from blunt chest trauma, typically affecting the right ventricle more commonly than the left ventricle because of its anterior location and proximity to the chest wall. The injury can range from mild bruising to severe myocardial damage and dysfunction.
It does not result from myocardial infarction (which is ischemic injury), nor does it cause hypertrophy or hypercontractility. Instead, it may cause wall motion abnormalities, arrhythmias, or even rupture.
These features are detailed in echocardiography and trauma cardiology literature, including the 'Textbook of Clinical Echocardiography' and clinical guidelines on blunt cardiac injury16:Textbook of Clinical Echocardiography, 6ep.600-60512:ASE Trauma Cardiology Guidelinesp.500-505.
Which method is appropriate for measuring the left atrial diameter in parasternal long axis?
Answer : A
Comprehensive and Detailed Explanation From Exact Extract:
The recommended method to measure left atrial diameter in the parasternal long axis view is the inner edge to inner edge technique, perpendicular to the aortic root, measured at end-diastole. This approach provides the most reproducible and standardized measurement.
Measurement parallel to the aortic root or at end-systole is less accurate. Outer edge measurements overestimate size.
ASE chamber quantification guidelines specify this method for standardization and reproducibility in adult echocardiography practice12:ASE Chamber Quantification Guidelinesp.90-9516:Textbook of Clinical Echocardiography, 6ep.120-125.
Which technique best determines a trileaflet aortic valve from a bicuspid aortic valve?
Answer : B
The most reliable technique to distinguish a trileaflet aortic valve from a bicuspid valve is to visualize all three leaflets simultaneously during diastole when the valve is closed. During diastole, the aortic valve leaflets coapt, and the three cusps form a characteristic ''Y-shaped'' or ''Mercedes-Benz'' sign on short-axis echocardiographic views, clearly demonstrating the number of leaflets.
Visualization during systole is less reliable because the valve is open, and the leaflets are moving rapidly. Doppler techniques (pulsed or continuous wave) assess flow velocities but do not definitively determine leaflet number, only stenosis severity.
This approach is well documented in adult echocardiography textbooks and ASE valvular imaging guidelines, which emphasize the diastolic short-axis view for valve morphology assessment16:Textbook of Clinical Echocardiography, 6ep.190-19512:ASE Valve Imaging Guidelinesp.180-185.