NAHQ Certified Professional in Healthcare Quality CPHQ Exam Questions
An orthopedic surgery practice has been working on Improving patient safety for the last 3 years. The following data table is available:
Which of thefollowing Is the most appropriate conclusion about patient safety outcomes?
Answer : D
Practice guidelines should be based on
Answer : A
Clinical practice guidelines (CPGs) are standardized recommendations to optimize patient care, and their credibility depends on a robust foundation of evidence.
Option A (Scientific evidence): This is the correct answer. CPHG guidelines must be grounded in scientific evidence, such as randomized controlled trials, systematic reviews, or meta-analyses, to ensure they reflect best practices. The NAHQ CPHQ study guide states, ''Clinical practice guidelines are developed based on scientific evidence to ensure they are effective and aligned with current standards of care'' (Domain 4). This aligns with organizations like the National Guideline Clearinghouse, which require evidence-based methodology for guideline development.
Option B (Computer-generated data): Computer-generated data (e.g., predictive analytics) may support decision-making but is not a primary basis for CPGs, which require peer-reviewed, clinical evidence.
Option C (Cost-benefit analysis): While cost considerations may influence implementation, CPGs prioritize clinical effectiveness and patient outcomes over financial metrics.
Option D (Utilization review criteria): Utilization review focuses on resource use and appropriateness of care, not the development of evidence-based guidelines.
CPHQ Objective Reference: Domain 4: Performance and Process Improvement, Objective 4.4, ''Support the development and use of evidence-based clinical practice guidelines,'' underscores that CPGs must be rooted in scientific evidence to ensure quality and standardization. The NAHQ study guide further notes that guidelines are typically developed by expert panels reviewing peer-reviewed literature to establish recommendations.
Rationale: Scientific evidence ensures CPGs are reliable, reproducible, and effective, aligning with the IOM's aim of effective care (delivering care based on best evidence). This distinguishes CPGs from other tools that may incorporate non-clinical factors.
A hospital collects patient satisfaction data by mailing surveys to patients discharged home and analyzes the responses they receive. What is the most significant limitation of this sampling methodology?
Answer : D
The most significant limitation of the sampling methodology in which a hospital collects patient satisfaction data by mailing surveys to discharged patients is the potential non-representativeness of the respondents. This can lead to biased results because:
Response Bias: The patients who choose to respond to the survey may have different experiences or opinions compared to those who do not respond. For example, individuals with very positive or very negative experiences may be more motivated to complete and return the survey, while those with neutral experiences may not bother to respond. This creates a response bias.
Nonresponse Bias: If a significant portion of the patient population does not respond to the survey, the data collected may not accurately reflect the overall patient satisfaction. This can result in an overestimation or underestimation of patient satisfaction levels, leading to incorrect conclusions and potentially flawed quality improvement strategies.
Sampling Bias: Since the survey is voluntary, there is no guarantee that the sample of respondents is representative of the entire discharged patient population. Factors such as age, literacy, socioeconomic status, and health condition might influence who responds, further skewing the results.
Impact on Data Validity: The lack of representativeness can compromise the validity of the findings. Decision-makers relying on these survey results may implement changes based on incomplete or biased information, which might not address the needs or concerns of the broader patient population.
NAHQ White Paper on Patient Satisfaction Surveys.
Quality Management in Health Care, Discussion on Sampling Methodologies.
NAHQ CPHQ Study Guide, Chapter on Data Collection and Analysis.
Survey preparation is initiated by a quality professional for an organization's annual three-year accreditation. The executive committee and department managers are given an organizational schedule for training and accreditation activities. Which of the following is the best tool to use to manage this initiative?
Answer : A
Managing an accreditation survey preparation initiative requires a tool to organize tasks, timelines, and dependencies across multiple stakeholders.
Option A (Gantt chart): This is the correct answer. The NAHQ CPHQ study guide states, ''A Gantt chart is a project management tool that sequences tasks, shows timelines, and tracks dependencies, making it ideal for managing complex initiatives like accreditation preparation'' (Domain 4). It visualizes the schedule for training and activities.
Option B (Multi-voting method): Multi-voting prioritizes options, not suitable for scheduling tasks.
Option C (Affinity diagram): Affinity diagrams organize ideas, not manage project timelines.
Option D (Ishikawa diagram): Ishikawa diagrams identify causes, not manage initiatives.
CPHQ Objective Reference: Domain 4: Performance and Process Improvement, Objective 4.3, ''Use project management tools,'' includes Gantt charts for initiative planning. The NAHQ study guide notes, ''Gantt charts are effective for managing accreditation preparation schedules'' (Domain 4).
Rationale: A Gantt chart ensures clear task sequencing and tracking, aligning with CPHQ's project management principles for accreditation.
The chart below reflects the 12-week period following implementation of a new electronic health record (EHR) at an outpatient clinic.
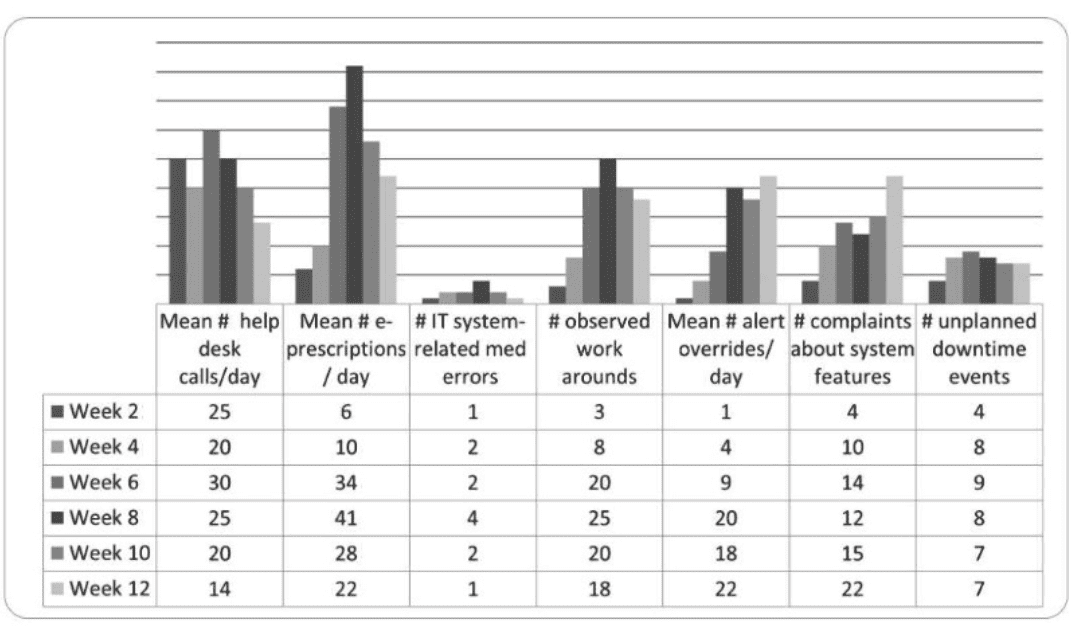
Based on the information above, which of the following conclusions can be drawn?
Answer : D
Implementing a new electronic health record (EHR) system in an outpatient clinic often introduces challenges that impact patient safety and workflow. NAHQ CPHQ study materials emphasize that post-implementation evaluation should focus on identifying barriers to effective use, as these can undermine the system's benefits, such as improved medication safety and care coordination. Common metrics in such evaluations include system-related medication errors, help desk calls, downtime events, overrides, workarounds, and staff complaints, which reflect user experience and system performance.
Since the chart is not provided, I'll base the answer on typical CPHQ scenarios for EHR implementation. The options suggest the chart includes data on e-prescribing stability, system-related medication errors, help desk calls, downtime events, overrides, workarounds, and complaints. Option D, ''Overrides, workarounds, and complaints indicate there are underlying barriers to use,'' aligns with a common finding in EHR post-implementation reviews. Overrides (e.g., bypassing alerts), workarounds (e.g., using paper notes instead of the EHR), and complaints typically signal usability issues, such as a poorly designed interface, inadequate training, or system inefficiencies. These barriers can lead to errors, staff frustration, and reduced patient safety, requiring targeted interventions like workflow redesign or additional support.
Option A, ''While e-prescribing processes are now stable, additional training is needed to improve staff competency,'' assumes e-prescribing stability, which may not be supported without specific chart data showing consistent performance (e.g., no recent errors). It also assumes training is the primary issue, which isn't directly indicated without evidence of competency gaps. Option B, ''There is a strong positive correlation between system-related med errors and help desk calls,'' requires specific data showing a statistical correlation (e.g., both metrics trending together), which cannot be confirmed without the chart. Option C, ''Minimal IT-related med errors and downtime events indicate that the system has improved patient safety,'' assumes low error and downtime rates, but the presence of overrides, workarounds, and complaints (implied by option D) suggests ongoing safety risks, contradicting this conclusion. NAHQ emphasizes identifying and addressing barriers to EHR adoption to ensure patient safety, making option D the most likely conclusion based on typical post-implementation challenges.
According to the Institute of Medicine's (IOM) report, Crossing the Quality Chasm, which of the following is identified as one of the six aims for improvement?
Answer : C
The IOM's Crossing the Quality Chasm (2001) outlines six aims for improving healthcare: safe, effective, patient-centered, timely, efficient, and equitable.
Option A (Low costs): Low costs are not one of the six aims, though efficiency indirectly addresses cost by reducing waste.
Option B (Population-centered): Population-centered is not an IOM aim; patient-centered care focuses on individual needs, not populations.
Option C (Effective): This is the correct answer. NAHQ CPHQ study materials cite effective care---delivering evidence-based care that achieves desired outcomes---as one of the six IOM aims.
Option D (Coordinated): Coordinated care is a component of patient-centered or efficient care but is not explicitly listed as one of the six aims.
A team has identified that labeled cutting boards are needed in a kitchen to decrease cross-contamination. After a new process has been implemented, it is discovered that the labeled cutting boards are not being used. Which of the following is the next action the team should take?
Answer : D
When it is discovered that labeled cutting boards, which were introduced to decrease cross-contamination, are not being used, the next logical step is to determine barriers to compliance. This step is crucial for the following reasons:
Identifying the Root Cause: Before taking any corrective actions, it is important to understand why staff members are not using the labeled cutting boards. Barriers might include a lack of awareness, inadequate training, inconvenience, or resistance to change.
Addressing the Correct Issue: Without identifying the barriers, any action taken may not be effective. For instance, increasing monitoring or initiating discipline without understanding why the new process is not being followed could lead to frustration and further non-compliance.
Facilitating Improvement: Once the barriers are identified, targeted interventions can be developed. This might include additional training, revising the process for ease of use, or addressing any misconceptions about the importance of the change.
Ensuring Sustainability: By resolving the underlying issues that prevent compliance, the organization can ensure that the process improvement is sustained over time, leading to better outcomes.
NAHQ CPHQ Study Guide, Section on Change Management and Compliance.
Quality Management in Health Care, Article on Identifying and Overcoming Barriers to Compliance.